THE FUTURE OF CLINICAL TRIALS
FDA leader: ‘stockpiling’ could transform clinical trial system

In college, acting US Food and Drug Administration (FDA) commissioner Janet Woodcock majored in chemistry, with a significant course load in biology. She brought all that practical knowledge to more than three decades of service at the FDA, including a total of 24 years as director of the Center for Drug Evaluation and Research, and a stretch as deputy commissioner of the FDA.
Considering all that experience and expertise, it’s hard to argue she’s anything but highly qualified for her current job.
“I feel like everything I've done practically in my life helped prepare me for that for this next step,” Woodcock said.
Last year, Woodcock joined Operation Warp Speed, the public-private partnership headed by the US government to facilitate and accelerate the development, manufacturing, and distribution of COVID-19 vaccines, treatments, and diagnostics. As the therapeutic lead of the initiative, she gained additional perspective on how things looked from the top.
“That gave me a perch from the Health and Human Services (HHS) level to see how things fit together, so all of that has helped me in what I'm doing now,” she said.
When newly elected President Joe Biden tapped Woodcock to take the helm of the FDA as acting commissioner, the pandemic maintained its position as the agency’s main target.
“The number one priority was to maintain our COVID-19 response, at the level that we were doing or even improve it,” she told us. “We’ve gone through quite a bit, with the problems with the adverse events with the Janssen vaccine, then the pause, and then release of the pause, and so forth.”
The government’s efforts appeared to be paying off—as of May 15, the Centers for Disease Control (CDC) reports that the US has administered approximately 270.8m vaccine doses within the country’s borders. What’s more, Woodcock said, she’s overseen an effort to get FDA staff inspected, so important work like inspections could continue in the face of the pandemic.
While the COVID-19 has impacted the agency and its work, Woodcock says, the people working at the FDA are heartened by seeing the contributions they are making.
“The morale is relatively high with the staff because they are public health people and they stepped up to the plate when they were needed,” she said. “They're making a difference, but we are doing different activities to try and make sure morale is maintained.”
Other high-priority tasks include managing funds (including money coming in from the American Rescue Plan Act of 2021); efforts to increase maternal and infant health—such as Closer to Zero, an action plan to curb toxic chemicals in baby food; and stepping up food safety measures.
One area Woodcock sees as ripe for improvement is the clinical research system. Like Jennifer Byrne, Javara Research CEO, Woodcock has decades of experience in the life sciences, providing her with a unique perspective of what has worked in clinical trials—and what could use repair. For example, she said, she observed challenges with COVID-19 related research and trials from her leadership position with Operation Warp Speed.
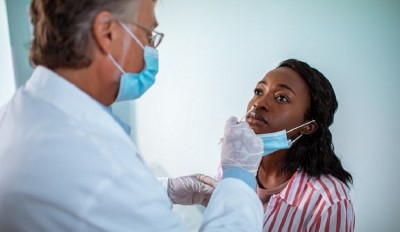
“One of the things we found when I was at therapeutics lead was that despite tens of thousands of people actually dying from the disease, and many more being hospitalized, we had trouble enrolling patients in trials, and we had trouble setting up sites,” she said. “Why? Who does trials in the US, and who sets up sites?”
While many public and private entities contribute to clinical research, Woodcock said, gaps in the infrastructure remain.
“There’s the National Institutes of Health, and federal granting programs—they set up sites and trials, they have networks, and the active programs they work with closely had done an inventory of all those very quickly so that they could be utilized,” she pointed out, adding that contract research organizations also offer preferred sites and highly trained, qualified staff for such research.
However, while the country’s healthcare system and institutions had scores of COVID-19 patients in their care, they lacked the resources needed to successfully conduct trials.
“Even with hospitals that are associated with universities that had trial sites didn’t have the training or the trial personnel,” she commented. “A hub university medical center couldn’t really enlist the surrounding hospitals in its system, even though they were full of COVID patients or COVID outpatients, because they didn't have the trained personnel and infrastructure available.”
Woodcock suggests creating a national “stockpile” of connected clinical trial infrastructure and resources. Similar to how countries like the US work to build up active pharmaceutical ingredients (APIs) and finished product in the event of shortages, a trial stockpile would serve to shore gaps in the nation’s clinical trial system by fixing the current disconnect between the trial and hospital system, and building a stronger connection between the two.
Earlier this year, Woodcock and FDA director for special programs Kevin Bugin co-authored an article in Nature, “Trends in COVID-19 therapeutic clinical trials,” which analyzed the global research landscape and found a number of concerning issues.
“What we found is that, if you applied pretty generous criteria to them, they had to be randomized and adequately powered, but only 5% of them were,” Woodcock pointed out.
One thing that the COVID-19 pandemic has revealed about issues with the clinical trial system, Woodcock explained, is the need for the country to have a better-prepared response plan in place before an event like a pandemic lands upon the country and becomes a calamity.
“You can’t build in time when a crisis is upon you,” she said.
With all the health conditions that need to be examined, drugs to be discovered, interventions to be studied, and more, Woodcock suggested, more qualified people should be enlisted in the cause. Bringing in the hospital staff, physicians, and other local-level care providers, she said, would help create the awareness, infrastructure, and community connections needed to strengthen the clinical research system.
“We need networks that are out in the community,” she said. “We need to train these folks—not every one of them, but enough people at community hospitals, federally qualified health centers, in rural areas, so if we have a pandemic or other crisis, they can be mobilized in the site and we can do large, simple trials and actually find out what to use quickly, what is the best treatment.”
In addition to creating a clinical research framework better braced for the next COVID-like crisis, Woodcock suggested forging a stronger connection with local care providers and promoting clinical resarch as a care option would help give participation rates for other trials a much-needed boost. For example, researchers currently estimate only 3% to 5% of cancer patients are presented with the option to participate in clinical trials.
“That's probably the opportunity to get the best treatment, to participate in a clinical trial, but most people aren't even offered,” she said. “I’ve been telling people we have to invest more in the infrastructure, keep it ‘warm’ or ‘hot’ on the off years when we're not having a crisis and studying all these other important things, and then we can rapidly transition it.”
Using the nation’s network of hospitals and healthcare systems, Woodcock suggested, would help create a clinical trial infrastructure and shorten the time needed to ramp up.
“It takes time,” she said. “That's what we mean by ‘stockpile’—you have to have that capacity and readiness; otherwise, it'll take you years to build up that capacity.”
In the next part of this series, Woodcock discusses the government’s role in supporting the clinical research industry, and ways the existing barriers to improvement could be eased.